Revenue Cycle Management
Managing healthcare’s revenue cycle is about more than collecting on unpaid bills. It’s about creating a positive and memorable experience for patients and employees. This consists of all administrative and clinical functions, and the various departments and staff that make up each patient’s unique healthcare experience. At RevCare Analytics, we do not just help health providers collect more, we guide them in transforming their revenue cycle from beginning-to-end. We specialize in transforming the financial health of healthcare providers through our expert Revenue Cycle Management (RCM) services. With a legacy of excellence, we ensure that every step of the revenue cycle is optimized for success.
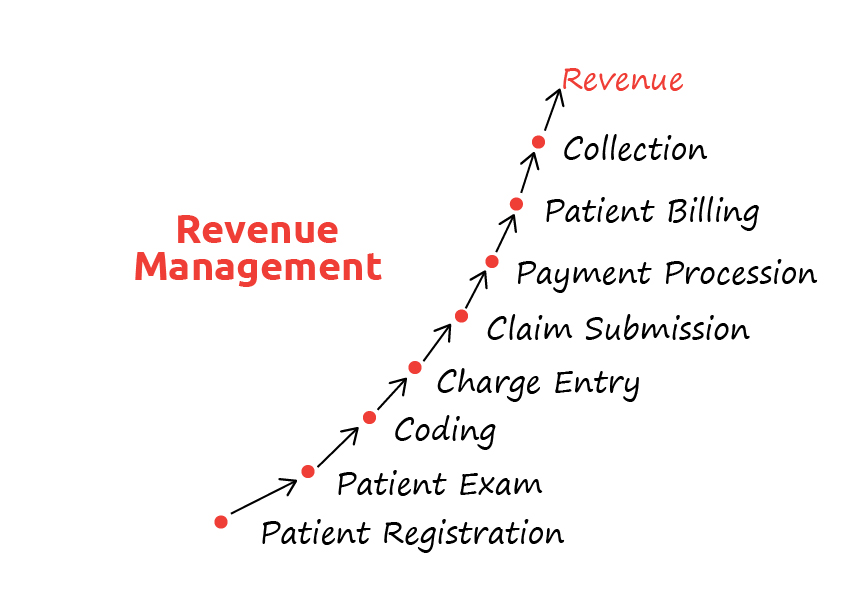
- Patient Registration
- Demographic and Insurance Verification
- Pre-Certification and Authorization
- Charge Capture
- Medical Necessity Checks
- Pre-Bill Edits
- Billing and Collections
- Legacy A/R Conversions
- Contract Compliance
- Denials Management: Technical and Clinical
- Payment Posting
- Patient Contact Center
- Self-Pay
- Reporting
- Government Reporting Management
- Credit Balances
Why RevCare Analytics?
- Proven Expertise: Our years of experience in healthcare billing have endowed us with a deep understanding of the RCM landscape, enabling us to navigate its challenges with expertise.
- Comprehensive RCM Services: We offer a full suite of RCM services, meticulously managing each aspect to ensure the financial vitality of your practice.
- Customized Approach: At RevCare Analytics, we recognize the uniqueness of each client. Our RCM solutions are tailored to meet the distinct needs of your practice.
Our RCM Services Explained:
- Patient Registration: The RCM process begins with patient registration, where we thoroughly capture all necessary patient demographics, insurance details, and other pertinent information. This foundational step is crucial for setting the stage for a smooth billing process.
- Insurance Verification: Our team conducts thorough insurance verification to confirm coverage and benefits eligibility. We obtain all necessary authorizations in advance, ensuring that services are appropriately billed and reducing the likelihood of claim denials.
- Medical Coding and Billing: Accurate medical coding and timely billing are the cornerstones of effective RCM. Our certified coders use the latest coding standards to ensure that every service rendered is correctly captured and billed, leading to a reduction in denials and an increase in reimbursements.
- Claims Submission: We diligently track each claim from submission to payment, engaging with insurance companies to resolve any issues promptly. Our proactive approach ensures that claims are processed efficiently, and payments are received in a timely manner.
- Payment Posting: Our payment posting services are accurate and timely. We accurately record all payments, adjustments, and denials into your system, always providing you with a clear financial picture. This transparency allows for better financial planning and analysis.
- Patient Billing: We handle patient billing with sensitivity and precision. Our team ensures that patients receive clear, accurate bills and statements. We also provide support for patient inquiries, helping to maintain a positive relationship between your practice and your patients.
- Accounts Receivable Management: Our accounts receivable management involves a strategic approach to monitoring outstanding balances and managing collections. We focus on improving cash flow by reducing days in accounts receivable and increasing the rate of collection.
- Business Intelligence Reporting: Data is at the heart of informed decision-making. Our business intelligence reporting services transform your raw data into actionable insights. We provide comprehensive reports on your practice’s financial performance, identifying trends and opportunities for improvement.
- Monthly Review Meetings with Practice: Collaboration is key to our approach. We conduct monthly review meetings with your practice to discuss financial performance, address any concerns, and strategize for the future. These meetings ensure that we are always aligned with goals and working towards your success.
The RevCare Analytics Advantage:
- First-Pass Claim Acceptance: Our expertise in RCM results in a high rate of first-pass claim acceptance, which means fewer claims are returned or denied, leading to faster reimbursement for your practice.
- Enhanced Revenue Collection: We are committed to recovering every dollar owed to your practice. Our meticulous attention to detail and relentless pursuit of outstanding claims result in increased revenue for our clients.
- Reduced Administrative Load: By partnering with RevCare Analytics, your staff can be relieved of the complex and time-consuming tasks associated with RCM, allowing them to focus on what matters most—patient care.
- Elevated Patient Satisfaction: A streamlined, and transparent billing process not only enhances the financial performance of your practice but also contributes to a better patient experience, leading to higher satisfaction and retention rates.
The advantages of RevCare Analytics technical expertise
- Grades of Service: RevCare Analytics offers a spectrum of services enhanced by technological innovation, from patient registration to billing and collections, ensuring a seamless and efficient revenue cycle management experience.
- Vendor Experience: With over 10 years of technology expertise, RevCare Analytics brings a wealth of knowledge and innovative solutions to healthcare billing, demonstrating adaptability and proficiency across various billing requirements.
- Pricing Guidelines: Leveraging technology, RevCare Analytics provides cost-effective solutions without compromising service quality, offering transparent pricing that aligns with client needs.
- Capacity & Infrastructure: The company’s robust IT infrastructure and team of experts ensure the capability to manage a large volume of claims and maintain the billing process for a diverse clientele.
- Service Level Agreements (SLAs): RevCare Analytics’ SLAs are backed by a commitment to technological advancement, ensuring reliability, data security, and consistent service performance.
- By focusing on these points, RevCare Analytics can effectively communicate its technical ability and the resulting operational excellence it brings to healthcare revenue cycle management.

RPA Services
Robotic process automation (RPA) is the use of software with artificial intelligence (AI) and machine learning capabilities to handle high-volume, repeatable tasks that previously required humans to perform. Once RPA software has been trained to capture and interpret the actions of specific processes in existing software applications, it can then manipulate data, trigger responses, initiate new actions and communicate with other systems autonomously.
- Data Entry tasks
- Payment Posting
- Automated Appeals
- Member Eligibility Checks
- Online Claim Status Checks
Contact Us
Contact us at info@revcareanalytics.com to experience the difference that RevCare Analytics can make for your revenue cycle workflow. We are not just about managing your revenue cycle; we’re about enhancing it. Our suite of services is designed to address every facet of the RCM process, ensuring that your practice thrives financially while delivering exceptional patient care.

